Epicardial patches are carefully engineered tissue patches that can be placed near or on a patient’s heart. These devices can help doctors to diagnose and treat a variety of heart conditions, including arrhythmia and heart attacks (i.e., myocardial infarctions).
In recent years, several engineers and medical researchers have been trying to develop these devices, yet many solutions proposed so far are not ideal. Specifically, most epicardial patches created so far are designed to be affixed onto the heart via a medical procedure known as “suturing,” which can be both challenging and risky.
Researchers at Sungkyunkwan University, the Institute for Basic Science and other institutes in South Korea recently developed an alternative epicardial patch that could be much easier to apply in clinical settings. This patch, introduced in Nature Electronics, is both stretchable and adhesive; thus, it does not need to be affixed onto a patient’s heart through the suturing process.
“The fixation of conventional epicardial patches to the heart tissue is a time-consuming task and involves a complex surgical process,” Prof. Donghee Son, one of the researchers who carried out the study, told Tech Xplore. “Furthermore, over prolonged periods of use, the durability of the flexible polymers composing the epicardial patch tends to degrade, leading to an undesired gap between the patch and cardiac tissue, ultimately making precise diagnosis and treatment difficult.”
To overcome the limitations of existing epicardial patches, lately some research teams have been experimenting with alternative designs based on soft biomaterials, such as glue or hydrogels. Despite some progress in this area, a reliable design has not yet been identified and commercialized.
“Considering the highly irregular surface of the heart, the existing devices with low adhesiveness often become detached due to continuous cardiac contraction/relaxation in long term,” Son said. “To overcome such issues, facile and instantaneous and even robust adhesion to cardiac tissues is essential. Furthermore, when attached to the heart for an extended period, the materials used in epicardial devices should be exceptionally soft to avoid causing any tissue compression.”
Son and his colleagues set out to develop a new adhesive epicardial patch that effectively overcomes the limitations of previously proposed designs. The patch they created can be instantly attached to tissue on the heart’s surface and could easily be fabricated on a large-scale.
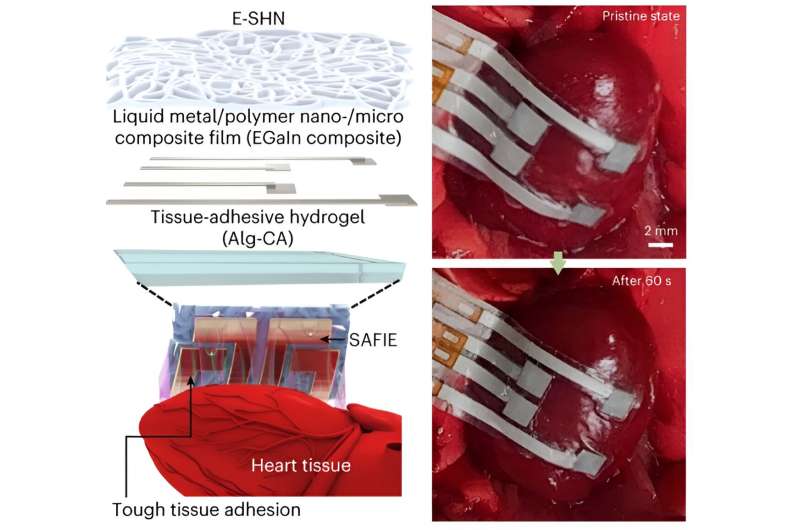
Notably, their patch does not exert any unnecessary pressure on the heart’s tissue for extended periods of time, which could improve both its safety and efficacy. It is comprised of three different but co-existing materials, namely a liquid-phase conducting composite, a network-shaped substrate, and an ionic adhesive.
The combination of these materials eliminates the need to suture the patch to the heart, making it easy to implement for medical professionals with varying degrees of experience, while also reducing the risk of complications associated with the suturing procedure.
“We designed the electronic patch with three layers consisting of soft, adhesive jelly-like materials known as hydrogels with ionic conductivity, stretchable electrodes made from liquid-phase metals, and fibrous-structured self-healing elastomeric materials, which are the key components of our innovation,” Son explained.
“Among them, the sticky hydrogels are inspired by the wet-resistant adhesion mechanism of marine mussels. The hydrogels play a crucial role by enabling immediate attachment of the entire electronic patch to the heart without the need for sutures.”
The adhesiveness of the team’s patch is further enhanced by its fibrous-structured substrate, which is designed to dissipate the mechanical stress spontaneously produced while the heart is beating. In contrast with other epicardial patches introduced in the past, the new device includes electrodes based on a liquid-phase metal, as opposed to solid-phase metals such as copper and silver.
“These liquid metal electrodes exhibit remarkable reliability and stability when monitoring epicardial signals, even under repeated heartbeats,” Son said. “We conducted experiments to record heart signals from awake and running animals for four weeks, marking a significant breakthrough.”
In addition to being safer and easier to apply to the heart’s tissue, the epicardial patch developed by Son and his colleagues can collect highly precise measurements, thus it can reliably diagnose heart attacks and arrhythmia, two of the most common cardiovascular diseases worldwide.
In addition, the patch can intervene on abnormal signals, modulating the heart’s rhythm and facilitating its normal functioning. As it is not as invasive as other patches introduced in the past, the team’s solution does not cause tissue damage or inflammation, reducing the risk of undesirable complications.
“Our intrinsically stretchable epicardial patch has electrical bidirectional functionalities that provide precise diagnosis and feedback therapy on cardiovascular diseases,” Son said.
“The patch can be instantaneously attached to heart tissues, leading to excellent prognosis. Our materials/devices strategy not only captures these diverse signals with precision but also has the capacity to locally stimulate tissues for therapeutic purposes, effectively functioning as an ‘electroceutical’ device. This dual functionality opens exciting possibilities for personalized medicine, where the patch can be tailored to an individual’s unique physiological needs.”
In initial tests, the epicardial patch developed by Son and his colleagues achieved highly promising results, highlighting its potential for advancing the diagnosis and treatment of heart conditions. The new solution could also have important implications for the field of precision medicine, allowing doctors to offer more personalized treatments tailored around the unique needs of individual patients.
“Our patch holds the potential to revolutionize the way we approach medical treatments, by combining the capabilities of signal recording and tissue stimulation,” Son added.
“We are currently in the process of developing an advanced bioelectronic patch with an expanded array of channels, surpassing the current limitation of four channels, this enhanced capability will enable us to monitor a wider range of electrophysiological signals, including those originating from electroactive tissues, peripheral nerves, skeletal muscles, and even the brain.”